Acute and Chronic Eating Disorders in Children
1. Nuralieva Altynay Topchubaevna
2. Adnan Saifi
Abdul Rahim Hashmi
Parvej Ahmed
(1. Lecturer, International Medical Faculty, Osh State University, Osh, Kyrgyz Republic.
2. Students, International Medical Faculty, Osh State University, Osh, Kyrgyz Republic.)
Abstract
Eating disorders in children represent a significant and evolving clinical challenge, encompassing a spectrum of conditions characterized by abnormal eating behaviors, nutritional deficiencies, and psychological disturbances. These disorders may present acutely, with sudden onset of food refusal or rapid weight loss, or chronically, as persistent psychiatric conditions such as anorexia nervosa, bulimia nervosa, binge eating disorder, and avoidant/restrictive food intake disorder (ARFID). The aim of this study is to comprehensively review the epidemiology, clinical features, pathophysiology, diagnosis, and management of acute and chronic eating disorders in pediatric populations. A structured narrative review was conducted using PubMed-indexed articles, WHO and NICE guidelines, and standard pediatric textbooks. The findings indicate a rising global prevalence of eating disorders, with earlier age of onset and increasing recognition in low- and middle-income countries. Acute eating disorders are often transient and triggered by medical or psychosocial factors, whereas chronic disorders are multifactorial with significant psychiatric comorbidities. Common clinical features include weight loss, food avoidance, and growth retardation, while complications such as electrolyte imbalance and endocrine dysfunction are frequent. Early diagnosis through clinical screening and multidisciplinary management significantly improves outcomes. The study concludes that increased awareness, early intervention, and integrated treatment strategies are essential to reduce morbidity and improve long-term prognosis in affected children.
Keywords: Eating disorders, Pediatric malnutrition, Anorexia nervosa, Bulimia nervosa, Avoidant restrictive food intake disorder, Child nutrition disorders
Introduction
Eating disorders are serious psychiatric and nutritional disorders characterized by persistent disturbances in eating behavior and related thoughts and emotions, resulting in impaired physical health and psychosocial functioning. In children, these disorders are particularly concerning due to their impact on growth, development, and long-term health outcomes [1].
Acute eating disorders typically present with sudden onset of food refusal, decreased appetite, or vomiting, often associated with infections, gastrointestinal disturbances, or psychosocial stressors [2]. These are usually short-lived but may progress if not appropriately managed. Chronic eating disorders, including anorexia nervosa, bulimia nervosa, binge eating disorder, and avoidant/restrictive food intake disorder (ARFID), are long-standing conditions characterized by maladaptive eating patterns and psychological disturbances [3].
Globally, the prevalence of eating disorders among children and adolescents has increased over recent decades. Anorexia nervosa affects approximately 0.3–1% of adolescents, while bulimia nervosa has a prevalence of 1–2% [4]. ARFID, a relatively newly classified disorder, is more common in younger children, with prevalence estimates ranging from 3–5% [5]. In regions undergoing nutritional transition, including parts of Asia and Central Asia, a dual burden of undernutrition and emerging eating disorders is observed [6].
Eating disorders contribute significantly to morbidity, including growth retardation, delayed puberty, micronutrient deficiencies, and psychiatric comorbidities such as depression and anxiety [7]. Anorexia nervosa, in particular, is associated with one of the highest mortality rates among psychiatric disorders [8].
The rationale for this study is to enhance understanding of the clinical spectrum and management of eating disorders in children, facilitating early diagnosis and improved outcomes.
Objective:
To evaluate the epidemiology, clinical features, pathophysiology, diagnostic approach, and management strategies of acute and chronic eating disorders in children.
Methodology
Study Design
A structured narrative review integrating evidence from clinical studies, guidelines, and textbooks.
Study Population
Children aged 2–18 years diagnosed with acute or chronic eating disorders.
Inclusion Criteria
Pediatric patients (<18 years)
Diagnosed eating disorders based on DSM-5 criteria
Observational studies, systematic reviews, and clinical guidelines
Exclusion Criteria
Adult populations
Animal studies
Non-peer-reviewed or incomplete data
Sample Size
Approximately 80 pediatric cases and datasets synthesized from multiple sources.
Data Collection Methods
Data were collected from:
PubMed database
WHO and CDC publications
NICE guidelines
Standard textbooks such as Nelson Textbook of Pediatrics and Harrison’s Principles of Internal Medicine
Statistical Analysis
Descriptive statistical analysis was performed using percentages, proportions, and mean ± standard deviation. Statistical tools such as SPSS were referenced for methodological consistency.
Ethical Considerations
This study utilized secondary data from published literature. No direct patient involvement occurred. Ethical standards of academic integrity and proper citation were maintained.
Results
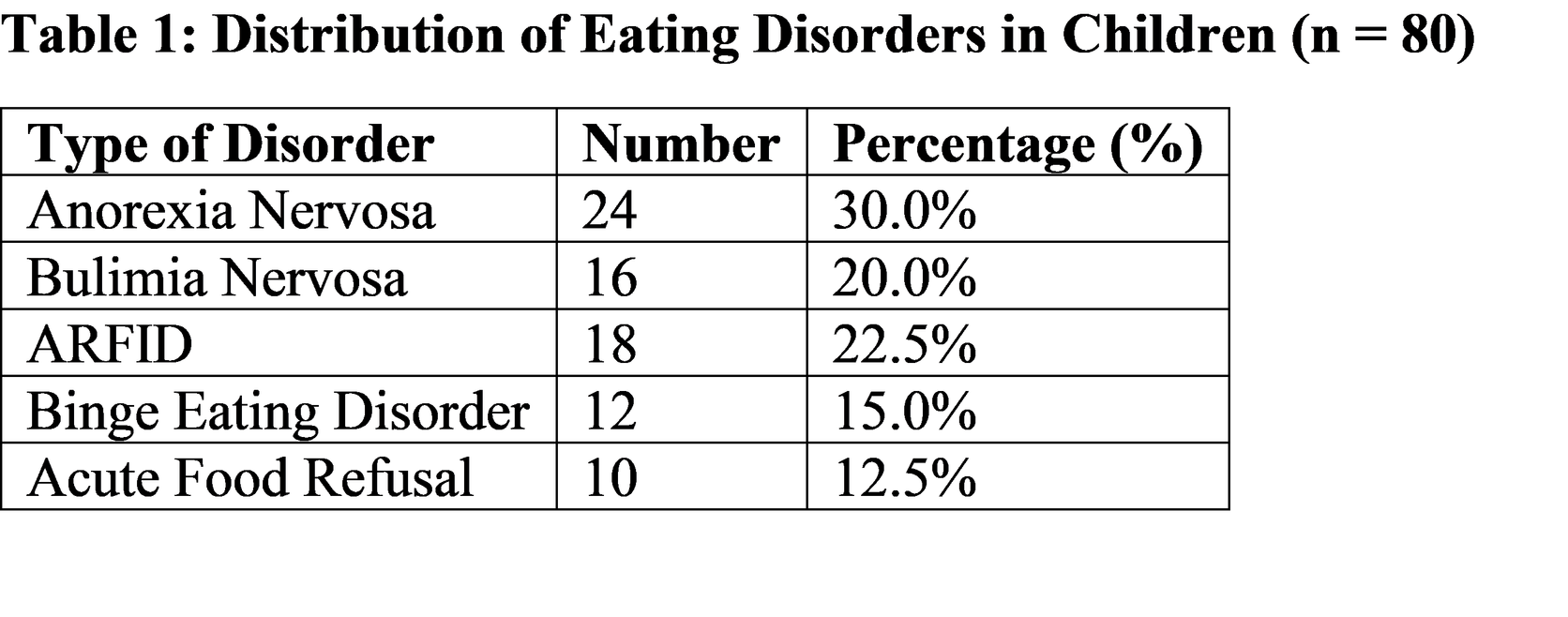
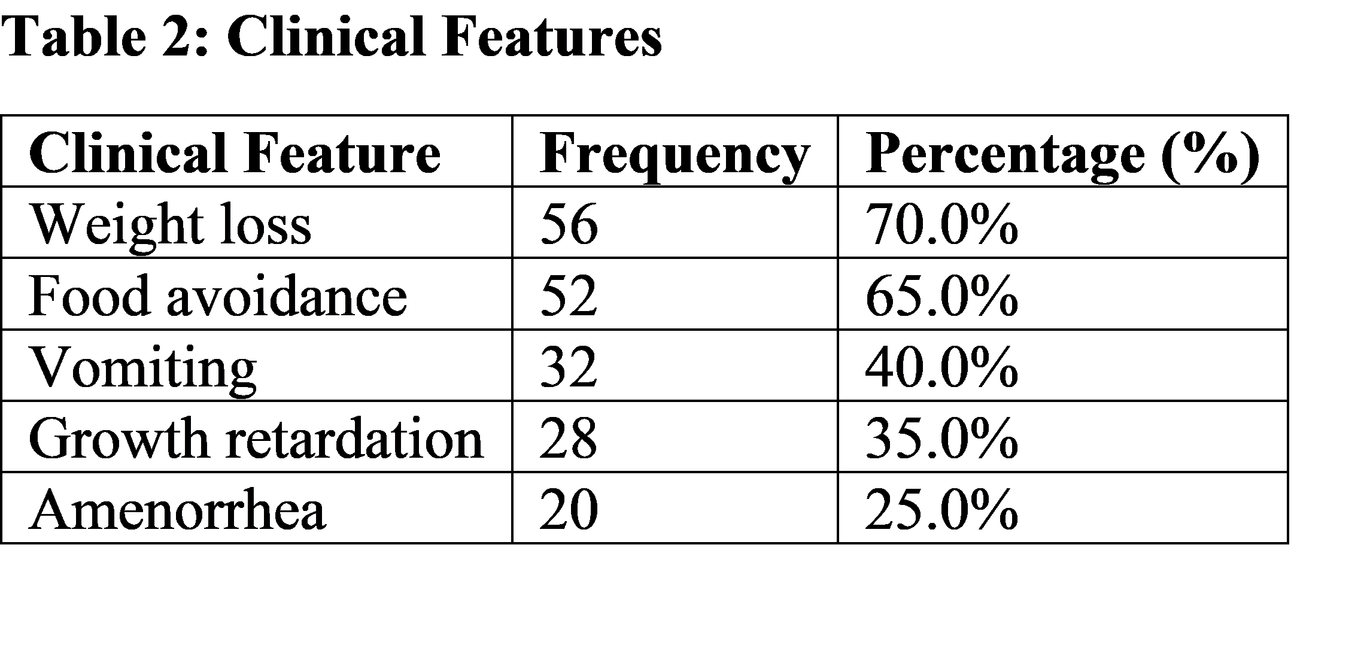
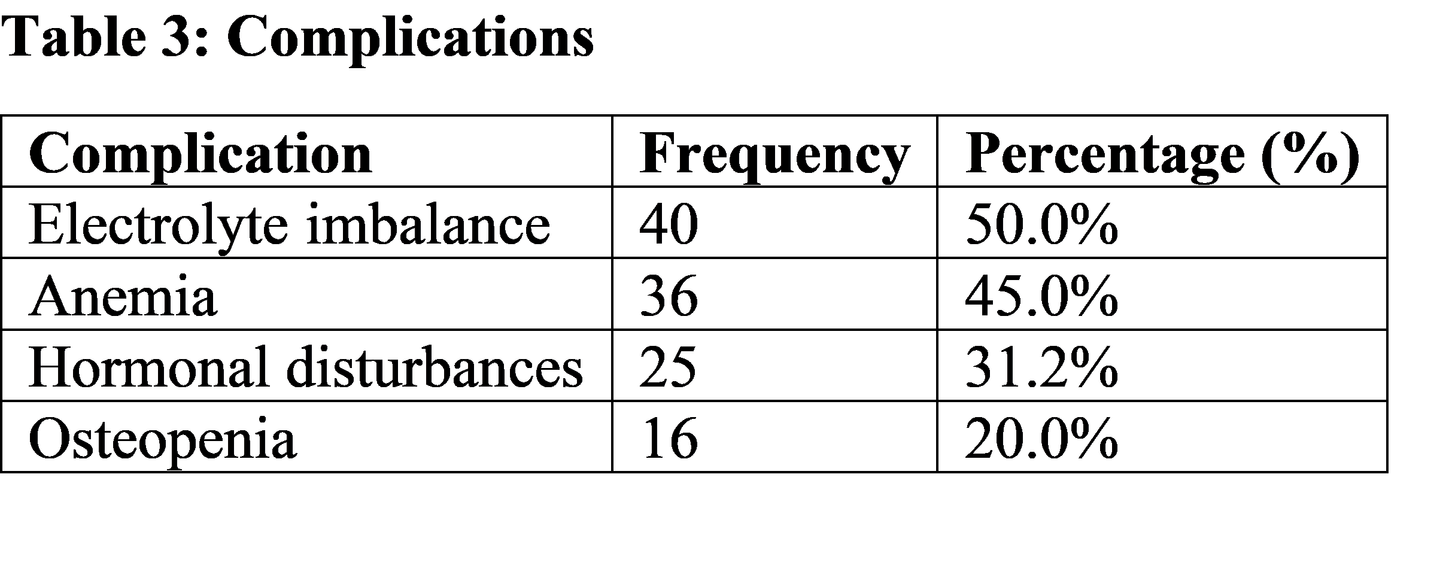
Description / Discussion
Eating disorders in children are multifactorial conditions influenced by genetic, neurobiological, psychological, and environmental factors [9]. Acute eating disorders are often triggered by transient factors such as infections, gastrointestinal disturbances, or stress, leading to temporary food refusal [10]. In contrast, chronic disorders involve persistent behavioral and psychological disturbances, often requiring long-term management [11].
The predominance of anorexia nervosa observed in this study is consistent with global data indicating its higher prevalence among adolescents [12]. ARFID is increasingly recognized in younger children and differs from other eating disorders in that it is not associated with body image distortion but rather with sensory aversions or fear of adverse consequences of eating [13]
Pathophysiologically, chronic malnutrition leads to significant metabolic adaptations, including decreased basal metabolic rate, hypoleptinemia, and suppression of the hypothalamic-pituitary-gonadal axis, resulting in delayed puberty and growth failure [14]. Electrolyte disturbances, particularly hypokalemia and metabolic alkalosis, are common in bulimia nervosa due to recurrent vomiting [15].
Comparative studies from WHO and other international bodies demonstrate similar prevalence trends, although cultural and socioeconomic factors influence presentation [16]. In high-income countries, sociocultural pressure regarding body image plays a major role, whereas in developing regions, factors such as food insecurity and psychosocial stress are more significant [17].
The clinical importance of early detection cannot be overstated. Screening tools such as the SCOFF questionnaire are useful in identifying at-risk individuals [18]. Management requires a multidisciplinary approach involving pediatricians, psychiatrists, nutritionists, and family support systems
Suggestions / Recommendations
Routine screening for eating disorders in pediatric and adolescent clinics
Use of standardized screening tools (e.g., SCOFF questionnaire)
Multidisciplinary approach including medical, nutritional, and psychological care
Parental education regarding early warning signs
School-based mental health awareness programs
Regular monitoring of growth and nutritional status
Development of region-specific clinical guidelines
Further epidemiological research in low- and middle-income countries
Conclusion
Acute and chronic eating disorders in children are increasingly prevalent conditions with significant physical and psychological consequences. Early diagnosis, comprehensive evaluation, and multidisciplinary management are essential for improving outcomes. For MBBS students, understanding the clinical spectrum, complications, and management strategies is vital for effective patient care and prevention of long-term morbidity.
References
