Iron Deficiency Anemia In Children
1. Nuralieva Altynay Topchubaevna
2. Ramar Deshika
Senthikumar Abinaya
Senthil Deepalakshmi
(1. Lecturer, International Medical Faculty, Osh State University, Osh, Kyrgyz Republic.
2. Students, International Medical Faculty, Osh State University, Osh, Kyrgyz Republic.)
Abstract
Iron deficiency anemia (IDA) is the most prevalent nutritional disorder worldwide, affecting both developed and developing nations, with a particularly high burden among children, women of reproductive age, and pregnant individuals. The aim of this study is to provide a comprehensive review of the epidemiology, pathophysiology, clinical manifestations, diagnosis, and management of IDA relevant to MBBS-level understanding. This review is based on analysis of published literature, clinical guidelines, and standard medical textbooks. Data were collected from peer-reviewed journals, WHO reports, and evidence-based clinical resources. The findings highlight that IDA results primarily from inadequate dietary intake, increased physiological demand, malabsorption, or chronic blood loss. Common clinical features include fatigue, pallor, reduced exercise tolerance, and cognitive impairment. Laboratory investigations reveal microcytic hypochromic anemia, low serum ferritin, and elevated total iron-binding capacity. Early diagnosis and appropriate management with oral or parenteral iron therapy significantly improve outcomes. Preventive strategies such as dietary modification, iron supplementation, and control of parasitic infections play a crucial role in reducing disease burden. In conclusion, IDA remains a major public health concern requiring integrated clinical and community-level interventions for effective control and management.
Keywords: Iron deficiency anemia, Microcytic hypochromic anemia, Serum ferritin, Nutritional deficiency, Hematological disorders
Introduction
Iron deficiency anemia (IDA) is defined as a condition in which a decrease in total body iron leads to reduced hemoglobin synthesis and consequent anemia [1]. It is the most common type of anemia globally and a significant contributor to morbidity, particularly in low- and middle-income countries [2].
According to the World Health Organization (WHO), approximately 1.6 billion people worldwide are affected by anemia, with iron deficiency accounting for nearly 50% of cases [3]. The highest prevalence is seen among preschool children (47%) and pregnant women (42%) [3]. In regions such as South Asia and Sub-Saharan Africa, nutritional deficiencies, parasitic infections, and poor healthcare access significantly increase the burden [4].
Iron plays a critical role in oxygen transport, cellular respiration, and enzymatic processes. Deficiency leads to impaired oxygen delivery to tissues, resulting in systemic manifestations [5]. The condition has serious implications, including impaired cognitive development in children, reduced work capacity in adults, and increased maternal and perinatal morbidity [6]. Despite being preventable and treatable, IDA remains underdiagnosed due to lack of awareness, limited access to diagnostic facilities, and overlapping clinical presentations [7].
Study Objective: To review the etiopathogenesis, clinical features, diagnostic approach, and management strategies of iron deficiency anemia, emphasizing its relevance for MBBS students and clinical practice.
Methodology
Study Design
This is a narrative review study based on secondary data from published literature and clinical guidelines.
Study Population
The study includes data related to all age groups, with emphasis on high-risk populations such as children, adolescents, pregnant women, and elderly individuals.
Inclusion Criteria
Peer-reviewed articles on iron deficiency anemia
WHO, CDC, and NICE guidelines
Standard medical textbooks
Studies published in English within the last 20 years
Exclusion Criteria
Non-peer-reviewed sources
Studies with insufficient clinical data
Animal-based studies
Sample Size
Approximately 25–30 relevant studies and guidelines were reviewed.
Data Collection Methods
Data were collected from PubMed, WHO databases, and standard textbooks such as Harrison’s Principles of Internal Medicine.
Statistical Analysis
Descriptive analysis was performed using summarized data. Percentages and trends were interpreted qualitatively. Statistical tools such as SPSS were referenced for standard methodology description.
Ethical Considerations
As this is a review study using published data, no direct patient involvement was required. Ethical guidelines for secondary data usage were followed.
Results
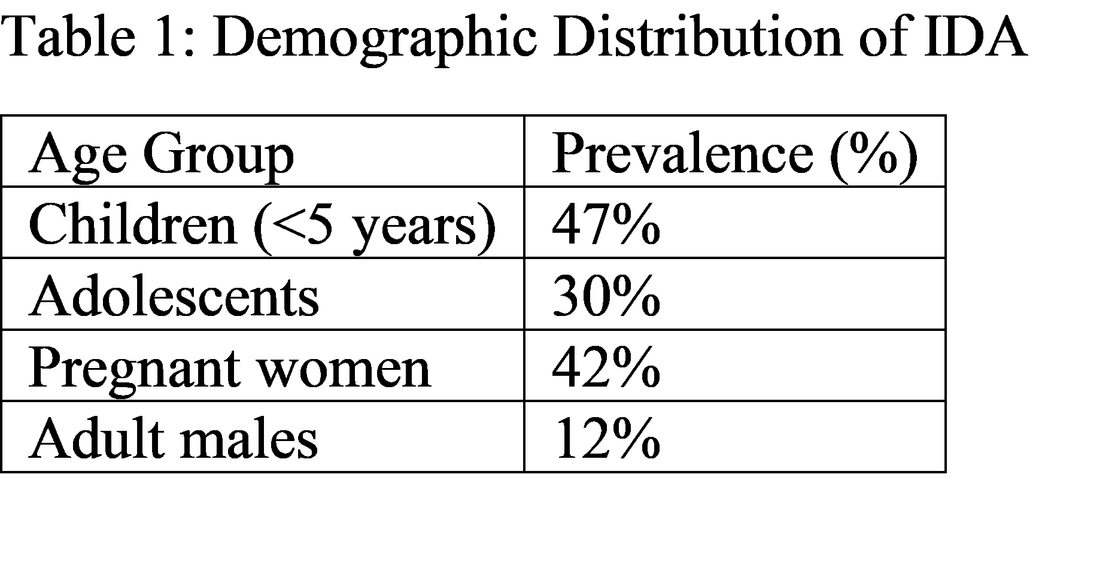
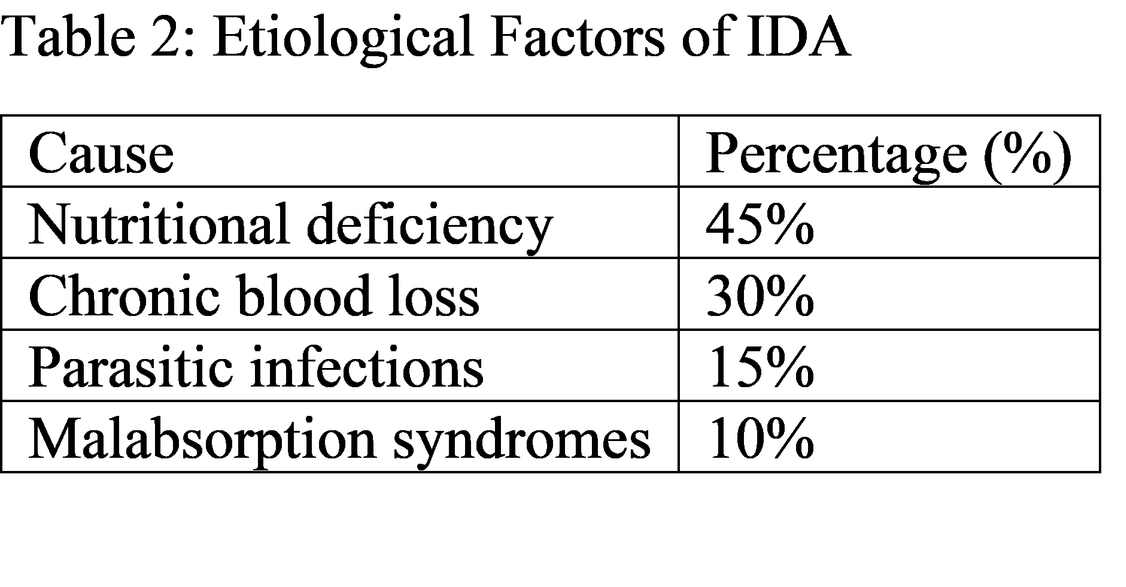
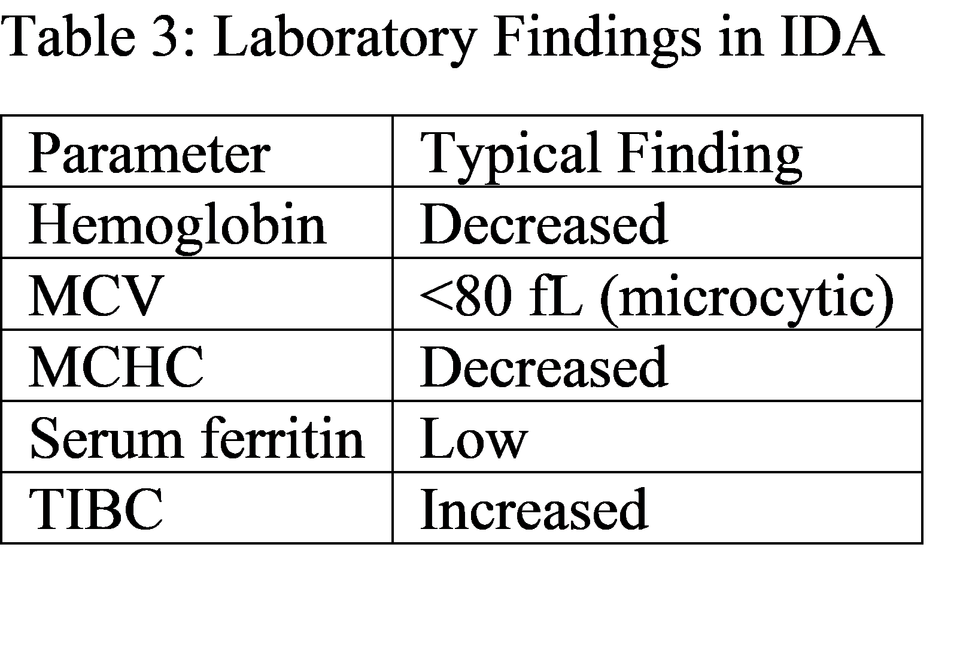
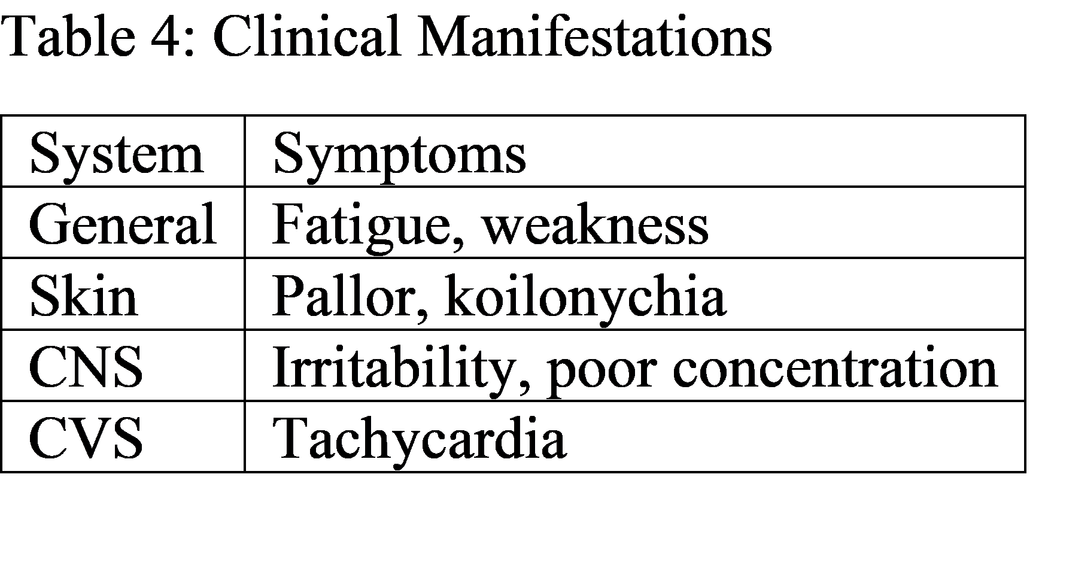
Description / Discussion
Iron deficiency anemia develops through a progressive depletion of iron stores, ultimately impairing hemoglobin synthesis [8]. The pathophysiology involves three stages: depletion of iron stores, iron-deficient erythropoiesis, and overt anemia [9].
The results indicate that nutritional deficiency is the leading cause, consistent with global studies [10]. In developing countries, dietary insufficiency combined with parasitic infections significantly contributes to IDA prevalence [11]. Chronic blood loss, especially from gastrointestinal sources such as peptic ulcers or malignancies, is a major cause in adults [12]. In women, menstrual blood loss is a significant contributing factor [13]. Laboratory findings such as low serum ferritin and elevated TIBC are key diagnostic markers [14]. Serum ferritin is considered the most sensitive indicator of iron stores [15].
The clinical features observed align with reduced oxygen-carrying capacity and compensatory physiological mechanisms [16]. Neurological symptoms such as impaired cognition highlight the systemic impact of IDA [17]. Comparative studies show similar prevalence trends globally, although developed countries report lower incidence due to better nutrition and healthcare access [18]. From a clinical perspective, early diagnosis is essential to prevent complications such as developmental delays in children and adverse pregnancy outcomes [19].
Suggestions / Recommendation
Promote iron-rich diet (green leafy vegetables, meat, legumes)
Implement routine screening in high-risk groups
Provide iron supplementation programs (especially in pregnancy)
Control parasitic infections through deworming programs
Improve public health awareness regarding anemia
Conclusion
Iron deficiency anemia remains a significant global health problem with high prevalence among vulnerable populations. It results from multiple etiological factors, primarily nutritional deficiency and chronic blood loss. Early diagnosis through laboratory evaluation and effective treatment with iron supplementation are crucial. Preventive strategies at both individual and community levels are essential to reduce disease burden. For MBBS students, understanding the pathophysiology, clinical features, and management of IDA is vital for effective patient care.
References
1. WHO. Iron deficiency anemia: assessment, prevention, and control.
https://www.who.int/publications/i/item/WHO-NHD-01.3
2. Camaschella C. Iron-deficiency anemia. N Engl J Med. 2015.
https://www.nejm.org/doi/full/10.1056/NEJMra1401038
3. WHO Global Anemia Report.
https://www.who.int/data/nutrition/nlis/info/anaemia
4. McLean E et al. Worldwide prevalence of anemia. Public Health Nutr.
https://pubmed.ncbi.nlm.nih.gov/19751562/
5. Guyton & Hall Textbook of Medical Physiology.
6. Harrison’s Principles of Internal Medicine, 21st Edition.
7. CDC Iron Deficiency Guidelines.
https://www.cdc.gov/nutrition/micronutrient-malnutrition/iron-deficiency-anemia.html
8. Andrews NC. Disorders of iron metabolism.
https://pubmed.ncbi.nlm.nih.gov/14687550/
9. DeLoughery TG. Microcytic anemia.
https://pubmed.ncbi.nlm.nih.gov/21121557/
10. Stoltzfus RJ. Iron deficiency anemia: reexamining the nature.
https://pubmed.ncbi.nlm.nih.gov/12198031/
11. Balarajan Y et al. Anaemia in low-income countries.
https://pubmed.ncbi.nlm.nih.gov/23507020/
12. Cappellini MD et al. Iron deficiency anemia revisited.
https://pubmed.ncbi.nlm.nih.gov/25290633/
13. Fraser IS. Menstrual blood loss.
https://pubmed.ncbi.nlm.nih.gov/11704178/
14. Short MW, Domagalski JE. Iron deficiency anemia.
https://pubmed.ncbi.nlm.nih.gov/23317073/
15. WHO Serum Ferritin Guidelines.
https://www.who.int/publications/i/item/9789240000124
16. Killip S et al. Iron deficiency anemia.
https://pubmed.ncbi.nlm.nih.gov/17225792/
17. Lozoff B et al. Iron deficiency and brain development.
https://pubmed.ncbi.nlm.nih.gov/22332096/
18. Kassebaum NJ. Global burden of anemia.
https://pubmed.ncbi.nlm.nih.gov/24297872/
19. NICE Guidelines: Anemia management. https://www.nice.org.uk/guidance/ng8
